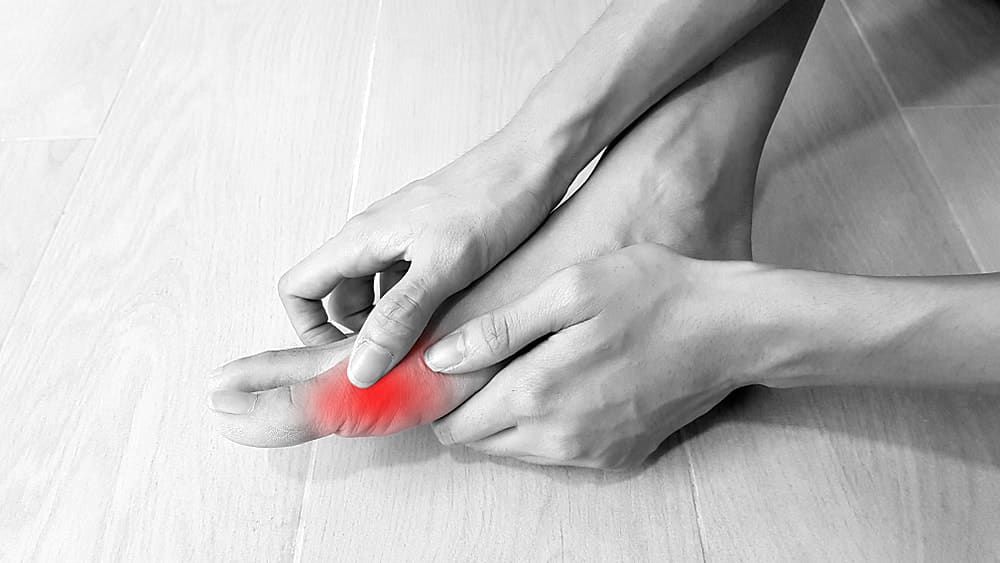
Although they are a very common condition. One of the more painful conditions to affect our feet are bunions.
A bunion is often described as the bony bump on the side of the big toe. The visual bump reflects changes in the bony structure of the forefoot.
Interestingly, the medical term for a bunion is ‘Hallux Abducto Valgus’ (HAV) — the term refers to the positioning of the toe, as it starts to turn inwards and overtime starts to move towards the lesser toes, creating a wider forefoot.
Bunions are a progressive condition, they start off small but can enlarge over time. And they can be symptomatic or asymptomatic in people depending on their severity.
If you’re experiencing pain from bunions, you’re at the right place. Let’s break down the symptoms, causes, treatments and prevention tips for bunions.
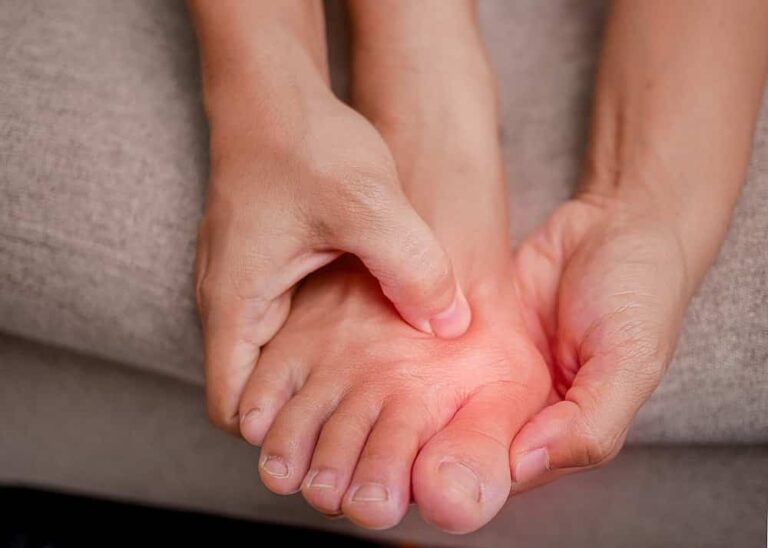
What Are The Symptoms Of Bunions?
Although bunions are not always symptomatic, they are a progressive disorder, which means they worsen over time.
They begin by a slight lean of the big toe towards the second toe. Some common signs and symptoms include:
- A bony bump developing on the inside or top of the big toe, which can become red and swollen
- Joint stiffness, loss of motion within the joint
- Deep, aching pain within the joint which worsens with footwear
- Difficulty fitting in shoes
- The second toe starting to become misshapen
Bunions can be classified into stages based on X-rays and degree of deformity:
Stage 1 (mild)
Stage 2 (moderate)
Stage 3 (severe)
Pain can occur at any stage. However, the more advanced stages are more commonly associated with pain and difficulty fitting into footwear.
As you can imagine, as the big toe drifts over closer and closer to the second toe, the bony bump on the side becomes larger, more painful and footwear options become more difficult.
Other forefoot complications also become more common as the smaller toes become impacted as well.

What Are The Main Causes Of Bunions?
A bunion forms when there is increased pressure and force placed on the big toe joint.
Some common causes include:
Gender. Females wearing tight or high-heeled shoes between 20 and 39 years of age have been found to have increased risk of developing bunions.
Familial Predisposition. Genetics plays a role in bunion development as bunions can run in families.
Tight Achilles Tendons. A tight Achilles tendon can alter the normal mechanics of the arch and forefoot leading to bunion formation.
Severe Flatfoot. This causes abnormal foot mechanics that may lead to the development of a bunion.
Systemic Disease. Disease such as arthritis can cause changes in the big joints which will alter the mechanics of the foot and cause a bunion.
The most common contributing factor is genetics. If you have noticed a bunion on your parent’s feet or even grandparents’ feet, chances are you have a higher chance of getting it.
Although the leading contributor, it is often a combination of all other factors as well.
The second biggest factor is footwear.
If you imagine your foot in a tight-fitting shoe, causing it to be squashed and in an awkward position where the toes are crammed together and the big toe joint naturally sticks out, this will cause permanent change over time within the joint, causing the big toe to move towards the second toe and your other toes to claw.
What Are The Available Bunion Treatments & Surgery Options In Singapore?
Some common treatments for bunions include:
Custom Orthotics to help offload areas that are being overloaded and worked, helping realign the foot and prevent the toe from further drifting inwards.
Exercises to help improve the strength of some of the smaller muscles around the joint.
Footwear Advice via assessing your footwear and give you appropriate advice to reduce bunion progression and pain.
Joint Mobilisation involves using hands-on therapy to help improve the joint range of motion.
Wearing Stable and Wider Shoes to help control foot movements and reduce pressure on the toes.
Ice Treatment for swelling and pain relief.
Medication for pain management and to reduce swelling.
Bunion Orthotics that limit pronation during toe off by redirecting to pressure away from the bunions.
Protective Padding to soften the pressure from the shoes.
If pain persists and you’ve exhausted all conservative treatment options, then it would be feasible for a surgical opinion.
Bunion surgery aims to bring your big toe back into its correct position and to relieve pain.
Several different surgical procedures have been used to treat bunions.
These include ‘shaving’ excess bone, removing the end of one of the bones or breaking and re-aligning the misplaced bone. Screws and pins are often used to hold the bones in their new positions.
What Are A Few Useful Bunion Prevention Tips?
Always ensure your footwear is correctly fitted and suitable for the activities you undertake.
Do not wear high-heeled shoes for long periods of time and for long distances.
Choose footwear that has adequate support and a retention mechanism (laces, velcro straps or buckles).
Keep track of the shape of your feet as they develop over time, especially if bunions run in your family and seek the advice of a an orthopaedic doctor early.
Let Us Help You With Bunion Treatments To Regain Your Quality Of Life.
Dr. Ananda Vella is a Singapore and Swiss-double-fellowship-trained MOH-accredited orthopaedic specialist consultant surgeon, As a former consultant from the Singapore General Hospital and Sengkang General Hospital and with more than 20 years of experience, Dr Ananda treats a variety of orthopaedic bone and joint conditions, including in his subspecialty focus of foot and ankle conditions, hip and knee pains, as well as sports injuries. Dr Ananda is also well-versed in minimally invasive surgical techniques, including having performed the first lateral total ankle replacement surgery in South-east Asia to improve outcomes for patients with severe arthritis.
Dr Ananda regularly practices in 3 clinics across Singapore and is accredited to operate in all private hospitals in Singapore. Should you have any queries or need any further assistance, please do not hesitate to schedule an appointment with our Dr Ananda by WhatsApp at 8860 0642 for assistance. Alternatively, please leave us a message via the enquiry form and we will get back to you as soon as possible.
(All Rights Reserved)